The human body relies on delicate systems to ensure seamless breathing and vital oxygen exchange. Within the chest cavity, a thin membrane called the pleura surrounds the lungs and lines the internal chest wall. Normally, a tiny amount of fluid lubricates these surfaces to prevent friction during respiration. However, when excessive fluid builds up in this space, a condition known as pleural effusion develops. This medical concern often signals an underlying health issue that requires prompt clinical attention and a thorough diagnostic evaluation.
Understanding the Mechanics of Pleural Effusion
To grasp the complexity of pleural effusion, one must first understand the anatomy of the pleural space. This narrow gap sits between the visceral pleura and the parietal pleura. Healthy bodies maintain a balance between fluid production and drainage through the lymphatic system. When this equilibrium breaks, fluid accumulates and compresses the lung tissue. Consequently, the affected lung cannot expand fully, which significantly impairs the patient’s ability to breathe comfortably.
The Two Primary Classifications
Medical professionals generally categorize pleural effusion into two distinct types based on the fluid's composition. Scientists use Light’s criteria to differentiate between transudative and exudative effusions.
- Transudative Pleural Effusion: This type occurs when systemic factors alter the hydrostatic or oncotic pressure in the body. Typically, the fluid is clear and low in protein. Common drivers include congestive heart failure or cirrhosis.
- Exudative Pleural Effusion: This variety results from local inflammatory processes or lung injuries. The fluid contains high levels of protein, cells, and enzymes. Pneumonia, malignancy, and pulmonary embolism often trigger this specific response.
Recognizing the Key Symptoms
Early detection of pleural effusion remains critical for successful management and recovery. While some small effusions remain asymptomatic, larger accumulations produce noticeable physical distress. Patients must monitor their respiratory health closely if they belong to high-risk categories.
- Shortness of Breath and Dyspnea: The most prevalent symptom of pleural effusion is dyspnea, or shortness of breath. As the fluid volume increases, it occupies space meant for lung expansion. Therefore, the patient feels a persistent sensation of air hunger. This breathlessness often worsens during physical exertion or when lying flat on the back.
- Sharp Chest Pain: Many individuals experience pleuritic chest pain, which feels like a sharp, stabbing sensation. This pain typically intensifies when the person takes a deep breath, coughs, or sneezes. Because the inflamed pleural layers rub against each other, the nervous system sends immediate distress signals.
- Persistent Dry Cough: A non-productive, dry cough frequently accompanies pleural effusion. The irritation of the lung lining or the compression of the airways triggers this reflex. Unlike a common cold, this cough does not resolve with standard over-the-counter suppressants.
Investigating the Common Causes
Identifying the root cause of pleural effusion is essential for determining the correct course of therapy. Because this condition is often a secondary manifestation, doctors must look beyond the chest cavity.
- Congestive Heart Failure: Heart failure stands as a leading cause of transudative pleural effusion. When the heart cannot pump blood efficiently, pressure builds up in the blood vessels. This pressure forces liquid out of the capillaries and into the pleural space.
- Respiratory Infections and Pneumonia: Infections represent a significant percentage of exudative cases. When bacteria or viruses attack the lungs, the resulting inflammation increases capillary permeability. Consequently, protein-rich fluid leaks into the surroundings, potentially leading to a parapneumonic pleural effusion.
- Malignancy and Cancer: Cancerous growths often interfere with the lymphatic drainage system. Lung cancer, breast cancer, and lymphoma frequently cause persistent pleural effusion. In these instances, the presence of malignant cells in the fluid confirms the advanced stage of the disease.
- Pulmonary Embolism: A blood clot in the lungs can also trigger pleural effusion. The clot disrupts blood flow and causes localized tissue damage or inflammation. Approximately one-third of patients with a pulmonary embolism will develop some level of fluid buildup.
Effective Treatment Options
The rising prevalence of conditions such as lung cancer, heart failure, and pneumonia has significantly fueled the expansion of the pleural effusion treatment market. Since pleural effusion commonly develops as a complication of these underlying diseases, it increases the demand for advanced diagnostic methods and effective treatment procedures, including thoracentesis and pleurodesis. Pleural effusion affects 1.5 million patients in the United States each year. The management of pleural effusion focuses on two goals: removing the fluid and treating the primary cause. Without addressing the underlying trigger, the fluid will likely return.
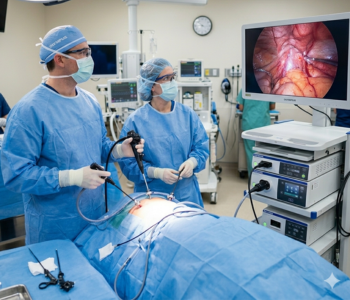
- Therapeutic Thoracentesis: For patients experiencing severe distress, doctors perform therapeutic thoracentesis to drain large volumes of liquid. Removing the fluid provides immediate relief from shortness of breath. However, this is often a temporary measure rather than a permanent cure.
- Medication Management: If heart failure is the culprit, diuretics help the body eliminate excess salt and water. Antibiotics are the standard treatment for pleural effusion caused by pneumonia. Similarly, steroids might reduce inflammation associated with autoimmune disorders like lupus or rheumatoid arthritis.
- Chest Tube Placement: In cases of recurring or infected pleural effusion, a surgeon may insert a chest tube. This tube remains in place for several days to ensure continuous drainage. This method is particularly effective for treating empyema, where pus accumulates in the pleural cavity.
- Pleurodesis: For chronic or malignant pleural effusion, doctors might recommend pleurodesis. This procedure involves injecting a chemical irritant, such as talc, into the pleural space. The irritant causes the two pleural layers to stick together, effectively closing the space where fluid accumulates.
Diagnostic Procedures and Evaluations
Clinicians utilize various tools to confirm a diagnosis of pleural effusion. Initially, a physical examination might reveal dullness to percussion or decreased breath sounds over the affected area.
- Imaging Techniques: Chest X-rays serve as the primary screening tool for detecting pleural effusion. If the X-ray shows a "meniscus sign," the doctor may order a CT scan. Computed tomography provides a more detailed view of the lung parenchyma and the pleural surface. Furthermore, ultrasound helps locate the exact pocket of fluid for safe extraction.
- Thoracentesis and Fluid Analysis: Thoracentesis involves inserting a thin needle into the pleural space to withdraw a fluid sample. Laboratory technicians analyze this sample for protein, glucose, pH, and cellular content. This procedure is vital for distinguishing between the different types of pleural effusion.
Conclusion: Prioritizing Respiratory Health
Living with pleural effusion requires a proactive approach to medical care and lifestyle adjustments. Understanding the symptoms allows patients to seek help before complications like lung collapse or sepsis occur. Because pleural effusion serves as a clinical red flag, thorough diagnostic testing is non-negotiable. By partnering with healthcare providers and following a structured treatment plan, individuals can manage the fluid levels and improve their quality of life. Always consult a medical professional if you experience persistent chest pain or unexplained breathlessness, as early intervention remains the cornerstone of effective pulmonary health.